The Nature of Melasma
Description
Melasma is a persistent skin ailment that is a multifactorial etiology that is influenced by a complex interaction of hormonal, genetic, and environmental variables. Melasma often appears as hyperpigmented spots on the forehead, cheeks, chin, and upper lip of the face, which are exposed to the sun. These spots frequently have wavy borders and range in hue from light to dark brown. Despite the absence of any physical symptoms, the illness can have a major negative influence on the standard of a person’s life and self-esteem.
You May Also Like:
CAN’T SLEEP? WHY NATURAL SUPPLEMENTS MAY BE THE ANSWER
IS THE NON ADDICTING SLEEP AID A MYTH? THE ANSWER MAY SURPRISE YOU.
Melasma: Description, Causes, And Treatment Protocol is an original (HealthXWire) article.
Possible Causes
There are many causes of Melasma. Although the precise etiology of melasma is still unknown, a number of possible causes have been noted, including the following:
Genetic Predisposition: A person’s vulnerability to melasma may be influenced by genetic factors. It usually runs in families, indicating a hereditary component. The way melanocytes react to environmental or hormonal cues may vary depending on certain genetic differences.
Hormonal Fluctuations: Hormonal changes have a profound impact on Melasma development. The disease is more common among women, particularly those who are pregnant, or using oral contraceptives. Elevated levels of both progesterone and estrogen during these times can encourage the production of melanin, resulting in the occurrence of Melasma.
Sun Exposure: Sunlight’s ultraviolet (UV) rays are known to cause Melasma. The skin’s pigment-producing melanocytes, which are activated by sunlight, can produce too much melanin, which leads to the development of dark patches. Melasma patients are more vulnerable to the development of hyperpigmentation because of their increased sensitivity to UV exposure.
Beauty and Skincare Items: Certain cosmetics and skincare items, particularly those that include strong scents, allergens, or harsh chemicals, may cause or aggravate Melasma. These items might irritate or inflame the skin, which would activate melanocytes and result in black spots.
Ethnicity: People with darker skin tones, including those people of Asian, Middle Eastern, Hispanic, and African origin, are more likely to develop Melasma. People who have higher melanin levels have more active melanocytes, which increases their risk of getting Melasma.
Exacerbating & Mitigating Factors of Melasma
The underlying factors of Melasma that are aggravating include:
Changing hormone levels: Hormonal changes can make melasma worse, including those that take place during pregnancy or when using oral contraceptives. Increased pigmentation is a result of how much progesterone and estrogen are present in the body.
Sun Exposure: A significant aggravating risk for Melasma is exposure to sunshine, particularly UV radiation. Melasma patches darken as a result of sunlight stimulating melanocytes and inducing melanin synthesis. Melasma that already exists may become worse by exposure to UV rays and may return.
Heat and Inflammation: Melasma can become worse if one is exposed to heat for a long time, whether it comes from hot showers, saunas, or the environment. Melasma patches might deteriorate due to inflammatory diseases, skin damage, or irritation.
Cosmetics and Skincare Items: The use of cosmetics or skincare products that contain irritants, potent fragrances, or harsh chemicals may exacerbate Melasma. Selecting cosmetics that are gentle on your skin is essential.
Certain Medications: Certain medications, including hormone therapies, antiepileptics, and specific photosensitizers, have been linked to Melasma. In persons who are vulnerable, these drugs may cause or exacerbate Melasma.
The melasma mitigation factors include:
Hormonal Management: For people who observe melasma flare-ups linked to hormonal shifts, managing hormonal triggers might prove advantageous. This could entail seeking non-hormonal treatments for menopausal symptoms or discussing alternate contraception methods with healthcare professionals.
Sun Protection: The management of melasma requires strict sun protection. This entails using a high-SPF broad-spectrum sunscreen, liberally slathering it on all exposed skin, alongside reapplying it frequently. Further protection may also be provided by physical barriers like sunglasses, hats, and clothes with a high UPF (ultraviolet protection factor) rating.
Inflammation and Heat Management: Melasma might improve if excessive heat exposure, is avoided. Melasma symptoms can be reduced by treating underlying inflammatory skin disorders like acne or dermatitis.
Gentle Skincare Regimen: Melasma sufferers must use moderate skincare items that do not aggravate their skin. Avoiding abrasive exfoliation, noxious odors, and harsh chemicals will help keep Melasma patches from getting worse.
Stress Management: While stress and Melasma have not been directly linked, reducing stress can benefit skin health in general. Melasma symptoms may be indirectly managed by performing stress-reducing activities like exercise and mindfulness exercises and getting advice from mental health practitioners.

Standard Treatment Protocol for Melasma
Topical medications, medical treatments, and dietary changes are frequently used in the treatment of Melasma. Based on the condition’s severity and unique patient variables, the specific method could change. Melasma is often treated with a combination of the following:
Sun Protection: Strict sun safety is the foundation of melasma treatment. This entails utilizing high SPF, i.e., 30 or higher, and liberally slathering them on all exposed skin. It is also crucial to wear protective clothing, including sunglasses and hats, and to find shade when the sun is at its peak.
Topical Agents:
- Corticosteroids
The effectiveness of other treatments can be increased by prescribing topical corticosteroids to decrease inflammation. Because of probable negative effects, they are normally utilized only briefly.
- Retinoids
Treatment of Melasma may benefit from topical retinoids like tretinoin. They function by accelerating cell turnover and hastening the fade away of hyperpigmented areas. Retinoids can be used independently or in conjunction with other substances.
- Hydroquinone
Topical Melasma medications frequently used include hydroquinone. It suppresses the formation of melanin. Between 2% and 4%, it comes in a variety of concentrations. Given the possibility of negative effects, prolonged use ought to be administered according to the supervision of a healthcare professional.
- Other Agents
Kojic acid, azelaic acid, tranexamic acid, and glycolic acid are additional topical treatments that could be employed. These substances function by reducing melanin synthesis or enhancing skin exfoliation.
Procedures:
- Microdermabrasion
An instrument that sprays tiny crystals or a wand with a diamond tip is used in microdermabrasion to remove the skin’s outermost layer. The physical appearance of Melasma can be improved by this process that helps eliminate dead skin cells.
- Chemical Peels
An acidic solution is used to scour away the outer layers of the skin during chemical peels. Melasma patches may be less noticeable and skin tone may even out as a result. Skin-deep peels, notably those that contain alpha-hydroxy acids, are widely used for managing Melasma.
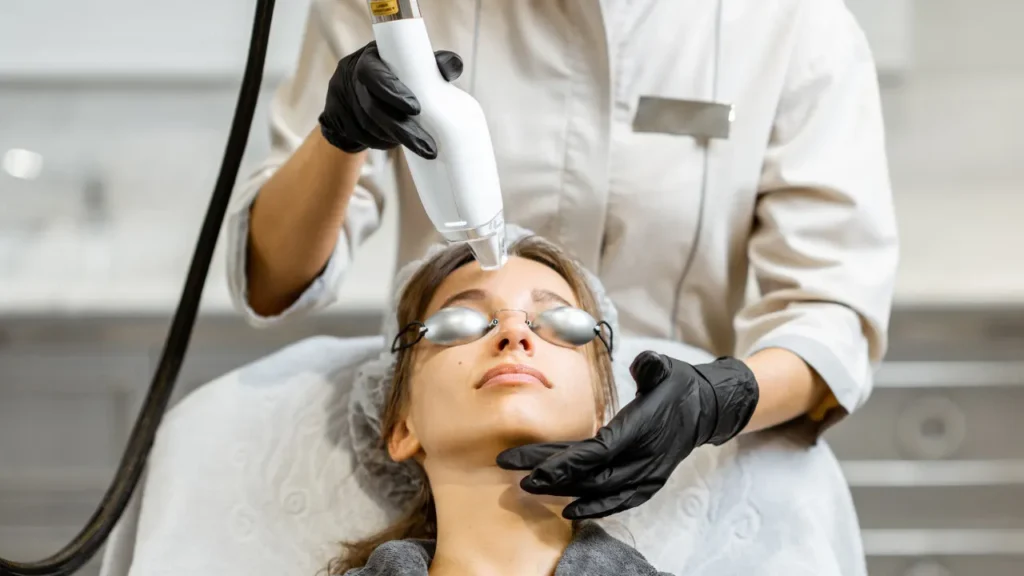
- Laser Therapy
Treatments using lasers, such as fractional laser therapy or intense pulsed light (IPL), can target and remove excess pigment from the skin. Usually, laser professionals or dermatologists carry perform these operations.

Lifestyle Modifications for Those Living with Melasma
- Hormonal Management
Discussing non-hormonal treatments for menopausal symptoms or other methods of contraception with women suffering from Melasma brought on or aggravated by hormonal changes might prove advantageous.
- Cosmetics
For those with Melasma, it is essential to select skincare and cosmetics which are non-comedogenic and not irritating to the skin. Preventing abrasive exfoliation, unpleasant odors, and harsh chemicals will help keep Melasma patches from getting worse.
- Medication Evaluation
It is crucial to discuss current medicines with a healthcare provider because some drugs can cause the onset or worsening of Melasma. When necessary, medication schedules should change.
Treatment Options for Those Living with Melasma
For the treatment of Melasma, a number of additional therapeutic options can be taken into account along with the usual procedure. These alternatives include:
Oral Medications: Oral medications can be prescribed as supplemental treatments for Melasma in some circumstances. Considerations could include oral contraceptives, tranexamic acid, and additional drugs that interfere with hormone regulation or melanin formation. With potential dangers and benefits in mind, these solutions should be evaluated by a medical expert.
Combination Therapy: When treating Melasma, combining various topical medications including corticosteroids, retinoids, and hydroquinone can increase their potency. Under the direction of a healthcare practitioner, this method should be used.
Natural and Herbal Remedies: Potential complementary therapies for Melasma have been investigated using several natural substances and herbal remedies. These involve substances like green tea extract, niacinamide, licorice extract, and vitamin C. They might show promise, but further studies are required to determine their safety and efficacy in curing Melasma.
Nutritional Supplements: Certain dietary supplements, like omega-3 fatty acids, polyphenols, and antioxidants, i.e., vitamins C and E, might be advantageous for the general health of the skin. Although they might not cure Melasma, they can maintain skin health and increase the effectiveness of traditional treatments.
However, the severity associated with the Melasma, medical history, skin type, and treatment objectives should all be discussed with a dermatologist or other healthcare provider to decide the best course of action for you. For optimal results, the treatment strategy should be customized to each patient’s particular requirements.


Melasma:
Conclusion
Melasma is a skin condition that can be brought on and exacerbated by a number of everyday factors. There are steps that a person with Melasma can take on their own and in consultation with a healthcare professional, such as a dermatologist, in order to treat this condition, which can persist if insufficiently treated. In addition to the physical effects of Melasma, this condition has the potential to affect people emotionally, as it often appears in places such as the face, neck, and head. Stay alert regarding changes to your skin and communicate changes or concerns to your doctor as soon as possible.


References:
- “Understanding Melasma.” Retrieved from: https://www.healthline.com/health/melasma
- “What is melasma?” Retrieved from: https://www.medicalnewstoday.com/articles/323715
- “Melasma: Diagnosis and Treatment.” Retrieved from: https://www.aad.org/public/diseases/a-z/melasma-treatment
- “Unmasking the causes and treatments of melasma.” Retrieved from: https://www.health.harvard.edu/womens-health/unmasking-the-causes-and-treatments-of-melasma
Important Note: The information contained in this article is for general informational purposes only, and should not be construed as health or medical advice, nor is it intended to diagnose, prevent, treat, or cure any disease or health condition. Before embarking on any diet, fitness regimen, or program of nutritional supplementation, it is advisable to consult your healthcare professional in order to determine its safety and probable efficacy in terms of your individual state of health.
Regarding Nutritional Supplements Or Other Non-Prescription Health Products: If any nutritional supplements or other non-prescription health products are mentioned in the foregoing article, any claims or statements made about them have not been evaluated by the U.S. Food and Drug Administration, and such nutritional supplements or other health products are not intended to diagnose, treat, cure, or prevent any disease.
Table of Contents


